Natural Family Planning - Is it Scientific? Is it Effective?
With the significant decline in infant mortality since the beginning of the 20th century, the need for child spacing became evident to many persons. In the second half of the 20th century non-coital contraceptives were discovered and assumed a high profile because they were aggressively promoted. Nevertheless, costfree natural methods are still preferred by many couples for reasons of economy, ecology, religion, as well as a desire to maintain control of one's own fertility.
Natural Family Planning
Definition
Natural family planning is planning for achieving or preventing a pregnancy by the timing of intercourse. By observing and recording certain natural symptoms and bodily changes that occur in a woman's menstrual cycle and using the information as a guide, a couple can learn to identify the fertile and infertile phases of the menstrual cycle. If the couple wishes to achieve pregnancy, they can be aware of the best days for this to occur. If the couple wishes to avoid pregnancy, they should abstain from intercourse or genital contact during the fertile or risk period of the cycle. Natural family planning for preventing pregnancy is also referred to as "periodic abstinence." The World Health Organization (WHO) defines periodic abstinence as voluntary avoidance of intercourse by a couple during the fertile phase of the menstrual cycle in order to avoid pregnancy.(1)
While the male is fertile from puberty onward, the female's fertile phase is recognizable by prospective and retrospective physiological markers, and normally occupies not more than one-third of the cycle.
The Hormonal Cascade of Ovulation
Prospective recognition of the fertile phase is based upon an understanding of the physiology of ovulation (Figure 1).
Figure 1
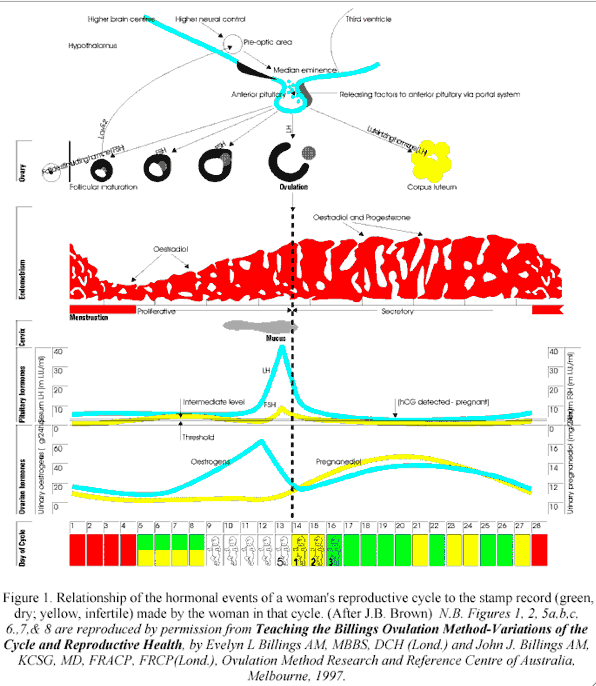
(end of figure 1)
At birth, the girl's ova are in the diplotene stage of development. They either remain quiescent or undergo atresia until puberty when some oocytes will mature and complete their meiotic division. The dominant follicle is selected within the first few days of the cycle by a rise in follicle stimulating hormone (FSH). FSH stimulates the granulosa of the healthy follicle to produce oestrogen and follicular fluid to form antral follicles. Oestrogen is produced by aromatization of androgens within the ovary. Antral follicles with the highest concentration of granulosal proliferation contain the highest oestrogen concentrations. These have the lowest androgen/oestrogen ratios and are most likely to house a healthy oocyte.
In the antral follicle, LH receptors are present only in the theca cells, while FSH receptors are present in the granulosa. LH stimulates the theca to produce androgens which can then be aromatised to oestrogens. Oestrogen exerts a negative feedback onto pituitary FSH production, which in turn causes withdrawal of gonadotropin support from the less well developed follicles which had begun to develop at the beginning of the cycle, causing a decline in their aromatase activity and limiting oestrogen production in those follicles. The dominant follicle reaches a maximum diameter of 19.5-25 mm prior to ovulation. The granulosa cells begin to acquire LH (luteinizing hormone) receptors.
Prior to ovulatory stimulation by LH, the concentration of oestradiol must be over 200 pg/ml and must be sustained for at least 50 hours until the LH surge has occurred. GnRH pulsatile release from the hypothalamus is present throughout the cycle, but is characterized by shorter pulse intervals and lower pulse amplitudes in the follicular, as opposed to the luteal phases of the cycle. Following ovulation or perhaps 24 hours prior to it, luteinization of the follicle produces progesterone, which in turn causes the well known conversion of endometrium to the secretory phase, suppresses cervical mucus with fertile characteristics (to be described subsequently), and when conjugated to pregnandiol, raises the basal body temperature.
The fertile phase of the female begins in the final ripening stage of the follicle when blood oestrogen level passes the threshold which triggers production of the different types of mucus from the cervical crypts. Prior to this event, the cervical canal has been protected and closed by a plug of tenacious mucus, the G mucus. (Figure 2).
Figure 2
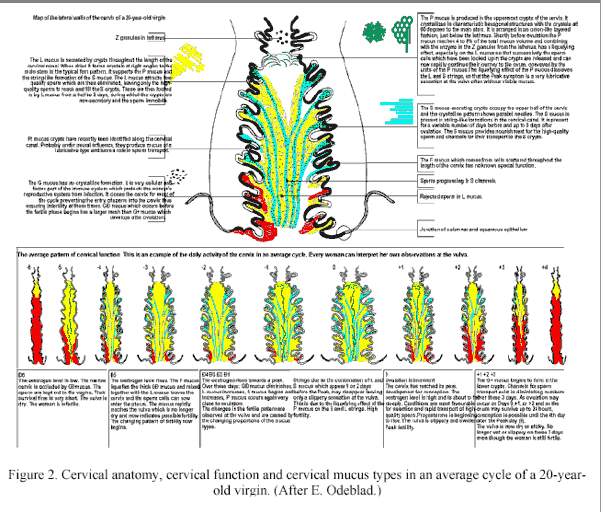
(end of figure 2)
When oestrogen rises, it stimulates the production of mucus from the L and S crypts which are located somewhat higher in the cervical canal. L mucus is slightly more fluid and initially dislodges the plug of thick mucus which then flows to the introitus. Women can both feel and see this without difficulty. L mucus is rather sticky, a bit elastic, and either opaque or translucent. Its function is to remove imperfect sperm forms and to close the opening of the S mucus crypts once these have been filled with (approximately) 20-30 spermatozoa. S mucus is more lubricative, elastic, and clear. It appears in strands, which actually conduct the sperm into the S crypts. There are 200-300 such crypts in the cervical canal. Each crypt can hold between 20 and 30 sperm. Once in the crypts, the sperm are nourished by the S mucus.
The opening of the crypt is closed by a plug of L mucus. Forty-eight to thirty-six hours prior to ovulation a surge of noradrenalin releases P mucus which comes in two forms. P2 dissolves the plug of L mucus allowing the sperm to emerge from the crypts and enter the central cervical canal, while P6 mucus strips prostaglandin F2 from the spermhead and provides additional energy for the journey into the uterine cavity and tubes. Around the time of the appearance of P mucus, the luteinizing hormone surge initiates the process of ovulation. The plasma oestrogen peak is followed usually in 1 to 36 hours by the LH surge. Ovulation follows within 17-36 hours of the LH surge. The fertilizable life of the ovum after ovulation is 8-12 hours.
Observation of the mucus sign is essential for recognizing not only the beginning of the fertile phase, but also for its ending. If oestrogen rises, the mucus becomes progressively more slippery, stretchy, and clear. Peak, which is defined as the last day mucus with fertile characteristics -- slippery, stretchy, or clear appears at the vulva. The largest amount of mucus, and the greatest elasticity (stretchiness) is met the day prior to peak. On peak, the P mucus makes the mucus so slippery and fluid that the amount and elasticity are reduced. Mucus is changed in its passage from the cervix to the vulva. Two structures parallel to the urethra, called the pockets of Shaw, contain manganese in their epithelium. The function of manganese is to absorb fluid from the vaginal canal. Oestrogen suppresses the function of manganese; hence, fluid can easily exit to the vulva when oestrogen dominates the cycle. After peak, L, S, and P mucus do not disappear immediately, but are no longer filled at the vulva because the fluid content has been reabsorbed.
Figure 3
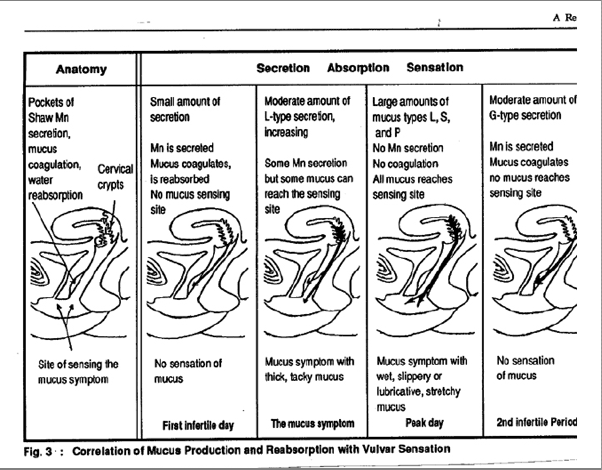
(end of figure 3)
This underlines the necessity of relying on external observations only when following the rules of the Billings Method. Eighty percent (80%) of women ovulate on peak day or the next day, 14% the day before peak, 3% two days before peak, and 3% two days after peak while a very small percentage - 0.3% have been found to ovulate on peak-3 or peak+3. Sperm are generally thought to be able to survive 48-72 hours in the cervical mucus. However, a longer sperm survival is occasionally encountered. This may be absolutely true or may be a combination of a longer sperm survival together with ovulation one or two days before peak. For all practical purposes, the fertile phase of the couple begins when the woman feels or sees mucus and ends the fourth day after peak.(3)
The cervix is a biological valve, and as such, is the gatekeeper for sperm to enter the uterus. Many investigators combined detection of cervical mucus at the vulva or at the cervix with temperature rise and calendar calculations to delineate the beginning and end of the fertile phase by multiple indices. Drs. John and Evelyn Billings pioneered the use of cervical mucus as a single parameter for the prediction of ovulation and its application to natural family planning. Women are taught to observe their mucus patterns at the vulva, relying primarily on the sensation of wetness and lubrication, obtained via ordinary sensation, augmented by the use of the Kegel exercise,palpation of the inner aspects of the labia minora with the finger, a "wipe-through" with toilet paper or a piece of cloth, or a combination of the above if needed. The mucus is then inspected for colour and is stretched to determine spinnbarkeit. According to Brown, whenever total oestrogens exceed the threshold of 15mg/100 ml/24 hours, the cervical mucus is sufficiently liquefied to leave the cervix and appear at the vulva.(5) If a cycle is ovulatory, the mucus will become increasingly lubricative, elastic, and clear until it reaches its "peak;" the changing behaviour of the mucus is called the mucus "buildup." "Peak" is defined as the last day of lubricative mucus, not necessarily the day of maximum stretch (elasticity).
When a cycle is ovulatory, the rising oestrogen level produces mucus in the cervical crypts. The first mucus found at the vulva is frequently the mucus plug which had closed the cervix after menstruation. The mucus plug is sticky, gummy mucus, which Erik Odeblad calls G mucus. It does not flow to the vulva until oestrogen has caused sufficient build-up of L mucus to dislodge it. Mucus is a hydrogel consisting of glycoproteins, water, chemical and biochemical compounds, including sodium, chloride, potassium, protein chains, and enzymes. They become polymers which change in response to type and level of the hormones acting on them.
Erik Odeblad has studied the cervical mucus since 1949 with nuclear magnetic resonance and spectrophotometry. He has demonstrated not only unique crystalline structure, but unique chemical compositions in each mucus. Figure 2 correlates the site of mucus production in the cervix with its appearance at the vulva. Fig. 2 also indicates how the crystalline structure of dry G, L, S, and P mucus would look.
G- mucus is produced in response to low levels of adrenal progesterone. After ovulation, G+ mucus is found in sufficient quantities to leave the cervix and be detectable at the vulva. Oestrogen rise initially triggers the production of L mucus which appears as loaf-like structures on the strands of mucus and selects out imperfect sperm forms. A higher level of oestrogen produces the S (or string) mucus which conducts sperm into the higher S crypts of the cervix. The S mucus nourishes the sperm in the crypts. P mucus is produced + or - 36 hours of oestrogen peak. Two forms of P mucus exist: P6 mucus, which conducts sperm cells from the S crypts into the uterine cavity and Pa mucus, which has a mucolytic function. It serves to open the barriers at the mouths of the S crypts and release the sperm at the time of ovulation. In addition, fetal cells which line the cervical canal produce a baseline discharge without lubrication, F mucus, in some women. As yet, no clinical significance has been discovered for F mucus.
Detection of the thermal shift via the daily basal body temperature (BBT) adds a retrospective confirmatory aspect. BBT is low until the event of ovulation, then rises .2-.3o C. When progesterone from the corpus luteum increases significantly it dominates the histology of the endometrium, changes the oestrogen-dominated proliferative phase to the progesterone-dominated secretory phase, and changes the lubricative oestrogen-induced mucus of the cervix to a sticky non-lubricative G mucus and when metabolized to pregnandiol, raises the BBT to produce the biphasic curve. Fig. 4.
Figure 4
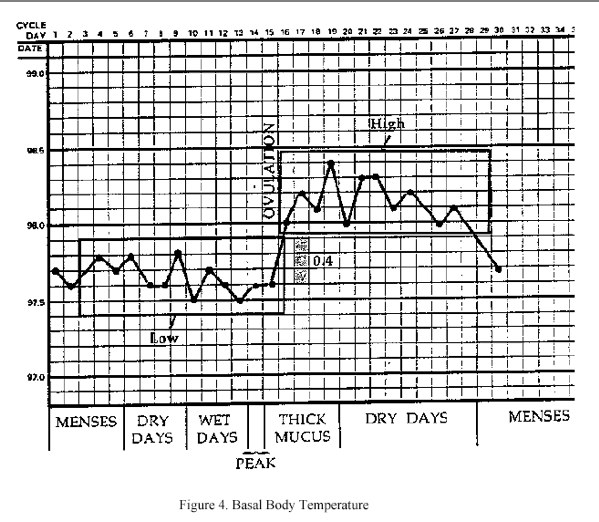
(end of figure 4)
History of Natural Family Planning
Even though women worldwide intuited that they were not always fertile, and sometimes correctly associated the mucus at the vulva with fertility, scientific investigation began with Von Baer's description of the mammalian ovum in 1827. Pouchet described intermenstrual pain and cervical mucorrhea in 1847; the biphasic temperature curve of women was first discovered in 1877 by Jacobi, but not conclusively related to ovarian activity until van de Velde's demonstration in 1905 and Hansen's in 1913. Clinical application of these findings were not made until the mid 1930s.
Calendar Rhythm
In 1903, Fraenkel had demonstrated that the life of the corpus luteum is 2 weeks. His findings were verified by Ogino in 1924, who described the normal luteal phase as 12 to 16 days long, and by Knaus in 1933, who reported that menstruation follows ovulation by approximately 2 weeks. An accurate history of the last 6 to 12 menstrual cycles is necessary to calculate the fertile and infertile phases of the cycle. Hartman calculated the fertile phase of the cycle by assuming a 12 to 16 day normal luteal phase, 72 hours for sperm survival, and 12 to 24 hours of ovum fertilizability. To estimate the fertile phase within the cycle, a woman with regular cycles needs to know the exact length of her last 6-12 cycles. She then subtracts 18 days from the shortest cycle to determine the last day of the early infertile phase, and subtracts 11 days from the longest cycle to find the last day of the fertile phase. Few women are "regular," but some have marked variations.
Calendar rhythm is generally credited with at least 20 per cent method failure. Roetzer has found that if one subtracts 20 days from the shortest cycle, rather than 18, the unplanned pregnancy rate is reduced; Roetzer uses the calculations in combination with cervical mucus and thermal shift (See Appendix). The use of calendar rhythm as an isolated method is not advocated by natural family planners, but it is still widely practiced, often by women who have an inadequate grasp on the necessary calculations, and still leads to many unplanned pregnancies.
In the Philippines, Laing found that the long-term unplanned pregnancy rates were similar for the pill and calendar rhythm (18 for both methods by 36 months), a figure which needs to be explained by the higher acceptability of calendar rhythm. Pill users were far more likely to discontinue the method.
Methodologies
Basal Body Temperature
Low basal body temperature in the preovulatory oestrogenic and slightly higher temperature in the postovulatory, progestational phase is a reliable indicator of the biphasic, ovulatory cycle. Various methods used to determine the onset of postovulatory infertility are described in the Appendix. A basal body temperature or a digital thermometer must be used. The same body orifice -- oral, vaginal, or rectal - - must be used throughout the cycle. The woman must have at least three hours of uninterrupted sleep prior to taking her waking temperature. She should take her temperature at the same time daily and use the same thermometer. Calibrations vary, so that if a thermometer is broken and a different one is used, the record may not be valid. Today few people use either the calendar or the basal temperature by themselves, because everyone agrees that the prospective sign of the cervical mucus is key for avoiding, as well as achieving pregnancy. When the granulosa cells of the cumulus oophorous of the follicle multiply rapidly, as they do just prior to ovulation, they produce interleuken 1. Interleuken 1 also raises the basal body temperature which could lead to error in determining the onset of postovulatory infertility.
The Symptothermal Methods
Several Western Centres have combined the prospective sign of the cervical mucus with the retrospective sign of the thermal shift after ovulation and with calendar rhythm calculations. Some systems, especially in parts of the U.S., have also added internal palpation of the cervix (See Appendix). Preference for a single or multiple index system depends on the availability of teaching and on the temperament of the learner. When either system is used correctly and consistently, results are comparable (See Effectiveness below).
Because the prospective sign of the cervical mucus is common to all methods, and is indispensable detecting the beginning of the fertile phase, it will be described in greater detail. The three most common symptothermal methods will be described subsequently.
The Billings Ovulation Method depends on self-detection of cervical mucus at the vulva by paying attention to how the vulva feels -- dry, sticky,or lubricated. The vulva can sense the presence of as little as 5 mg of mucus, while 40 mg of mucus are needed to obtain enough mucus for visual inspection. A woman is invited to observe for the presence or absence of mucus at the vulva prior to each act of urination and to record what she has felt and seen on a simple chart at the end of each day. (N.B. The Billings publications have generally avoided recommending specific times and places and techniques for making observations. The most recent Personal Record Chart Instructions state "As you go about your normal activities the sensations at the vulva can be identified". Ed.) If she is already sexually active when she is learning the method, she must refrain from sexual activity from the beginning of one cycle until she has experienced the changing mucus "build-up" pattern which leads to ovulation and to continue sexual abstinence until the fourth day after peak. The usually encountered build-up pattern is shown in Figure 5b. The fertile phase begins when mucus is detected at the vulva and continues until the fourth day after peak. Any intercourse or genital contact may lead to pregnancy during this time.
Figure 5a
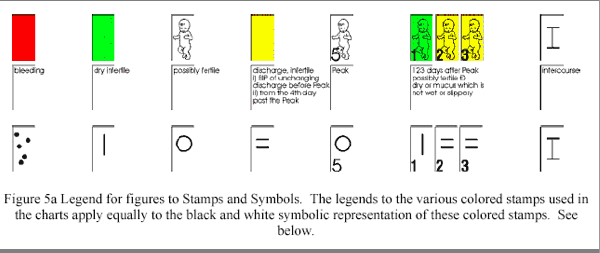
(end of figure 5a)
Figure 5b
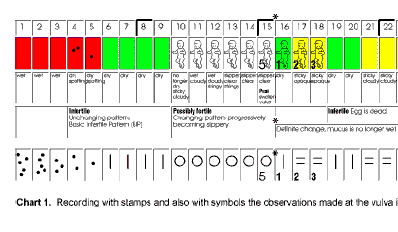
(end of figure 5b)
While the menstrual days as such are not necessarily days of fertility, nevertheless, most cultures avoid intercourse during menses. This serves the purposes of the Ovulation Method well as bleeding may obscure the beginning of mucus build-up prior to the end of menses in the case of a short cycle. It is known that sperm die rapidly - perhaps within 30 minutes - in the acid vagina, but may survive up to five days when the mucus is in its fertile phase. Dry days following menses then are not yet days of fertility. Couples wishing to avoid pregnancy may have intercourse on the infertile days; however, it is suggested that they restrict intercourse to alternate evenings in order to permit the woman to observe for the presence of mucus and also to avoid the confusion between seminal discharge or 'arousal fluid' (Bartholin gland secretion) and beginning mucus on the day following intercourse. Thus, alternate evenings of dry days are available during the early infertile days. When avoiding pregnancy, all the days of mucus until peak (the last day during which mucus is either slippery, stretchy, cloudy, or clear) and a full three days following peak are the fertile days of the couple. Once the mucus peak has been identified, it is followed by the luteal phase. Women generally have the same length of luteal phase each month. The normal range is 11-16 days. Once the peak rule of waiting until the fourth day after peak to resume intercourse has been observed, there are no further rules until the next period (see Fig. 5c and Appendix). Figures 5b & 5c show a typical ovulatory cycle recorded with colored stamps as well as the simpler symbols, which are used in many developing countries.
Figure 5c

(end of figure 5c)
If there is any bleeding or spotting other than menstruation, this is considered to be a sign of fertility, and is not available for intercourse, nor are the following three days until the evening of the fourth day. When a woman has a long cycle or a day or more of mucus which does not progressively change towards the more slippery, stretchy* variety, these are called patch patterns. [* "'stretch' and at other times as 'elasticity', neither of those words being appropriate to the observation of the mucus with fertile characteristics showing a tendency to form strings exactly as was originally described by the Germans with their word spinnbarkheit. It is the loss of any slipperiness or wetness that helps define the Peak and the tendency to form strings usually occurs, if at all two or three days before the Peak and ceases because of the mucolytic effect of the enzyme formed by a combination of zymogen granules from the isthmus of the cervix with the P-mucus.The same enzyme liberates sperm which may have been locked in the crypts by the L-mucus.The liberation of the G-mucus plug is also assisted by P-mucus working in combination with the L-mucus when the oestogen level begins to rise. (Personal correspondence from Dr. John Billings, September 26, 2000)]. Figure 6 shows such a cycle in which a typical "buildup" occurred. Later, peak was on day 46.
Figure 6
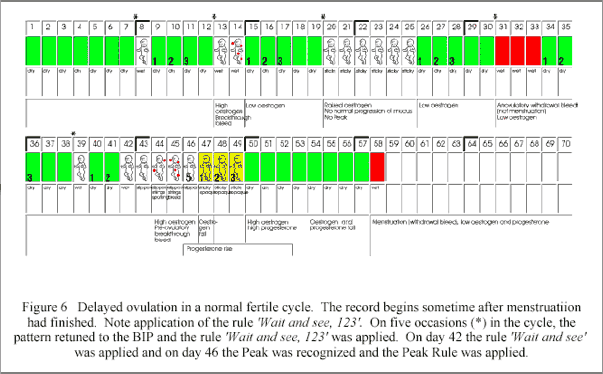
(end of figure 6)
Figure 7
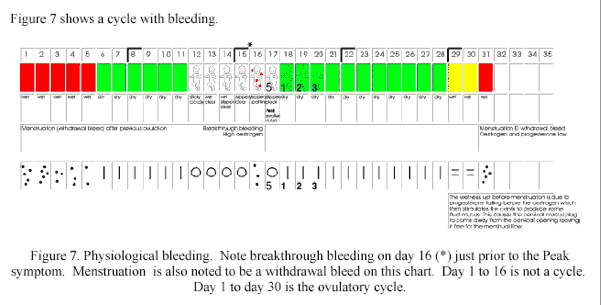
(end of figure 7)
Figure 8
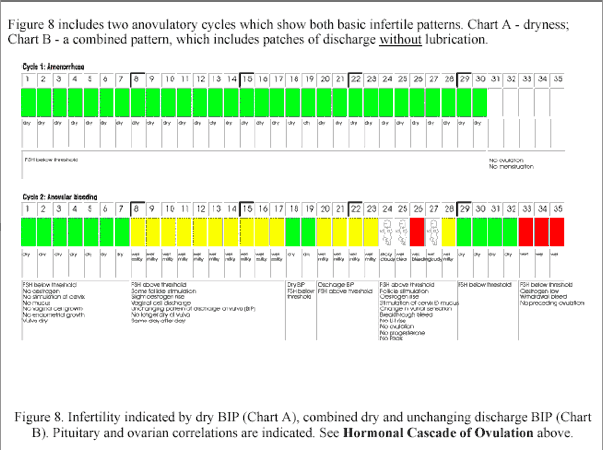
(end of figure 8)
A trained teacher is the best vehicle for correct instruction. The World Health Organization found that more than 90% of women could identify their cycle phases correctly in the first month of learning, the rest no later than by the third month. The mucus sign reflects the rising oestrogen of the ripening follicle and gives warning of the beginning of the fertile phase in all reproductive situations. The method has been applied successfully, not only during regular and irregular cycles, but during breastfeeding, premenopause, cessation of anovulant medication and during puberty.
Modifications of cervical mucus methods
To make natural family planning more attractive to potential acceptors by reducing the days of necessary abstinence, K. Dorairaj, who works mostly with very poor, uneducated, and poorly nourished women in India, has adapted the Billings rules: the women do not chart their observations, do not follow the "early day rule" which restricts intercourse to alternate evenings of the early infertile days of the cycle and wait only two days after peak day to resume intercourse. Comparative studies found somewhat higher rates of unplanned pregnancy and lower continuation rates than the Billings method.
Another modification was introduced at Creighton University in Omaha, Nebraska. It utilizes a standardized nomenclature to describe mucus observations, has modified several rules and considers any pregnancy as planned if conception occurred after the first three months of instruction from an act of coitus during a time of recognized fertility. Thus comparison of unplanned pregnancy rates as defined by other methodologies is not possible.
Anovulation
Oestrogen withdrawal bleeding in the absence of ovulation is encountered frequently in early puberty, after childbirth, when beginning weaning as well as after weaning, during premenopause, and upon discontinuation of anovulant medications, either oral or injectable. In those situations, the temperature pattern is monophasic, while the mucus pattern displays only patches of mucus with fertile characteristics, usually without a proper buildup to peak and with either breakthrough or withdrawal bleeding. In addition, the number of days which follow the last day of mucus seldom equal those of a normal luteal phase, being either shorter or longer. Only 50% of cycles are ovulatory in the first year of menses are ovulatory cycles. This increases by 10% each year until the woman is five years past menarche, when 85% of cycles are ovulatory. Even at the peak of fertility, women do not ovulate every month. In the face of stress, rapid weight loss, or rapidly increasing athletic training, anovulatory cycles are frequently encountered.
Lactation
Full lactation suppresses FSH and LH initially because of the high prolactin level, but amenorrhea may very well persist even when prolactin drops because the hypothalamo-pituitary ovulatory cascade is disrupted. When using the ovulation method or sympto-thermal methods, the woman is instructed to observe for the return of any signs of mucus, either by sensation or visual observation, and to presume that fertility is returning when signs are encountered. It is not uncommon to encounter a thin gray nonlubricative discharge during full lactation because of (physiological) atrophic vaginitis. This is different from mucus which has body and lubrication, or at least a rubbery consistency and elasticity. Once signs of fertility are encountered, the woman initiates the rules of the method.
The lactational amenorrhea method (LAM) is now being used in a number of countries, mostly through World Health Organization efforts. The Bellagio Consensus found that if women are still amenorrheic when the baby is six months old, and they are fully nursing, i.e., giving the baby only the breast, no top feeds, no fluids, except for an occasional taste of food, the woman had only a 2% risk of pregnancy.(6) At such time, she is invited to consider a transitional method. Many women do not fully breastfeed for six months, while other women return to menstruation and ovulation at 90-180 days postpartum. The "short amenorrhea" group has lower biologically active (BIO-PRL) prolactin than immunoreactive (IR-PRL) levels, while the "long amenorrhea" groups exhibit higher BIO-PRL levels. Unless one is able to screen for BIO-PRL/IR-PRL ratios, it is highly advisable to invite women to begin to observe for signs of mucus as soon as the lochia stop. In that way, they will not be surprised by the return to fertility.
Premenopause
The mucus sign is the most useful sign in premenopause. As the cervix ages, squamous epithelium begins to extend into the endocervix, the G mucus bearing area is found higher in the canal and the areas which produce L and S mucus gradually decrease; the number of days of mucus with fertile characteristics are reduced. Odeblad has shown that between ages of 13-17, the average woman has 8 days of mucus of which 6 are slippery (S mucus), while by age 33-37, the total days of mucus are 4.8 and less than 2 are slippery. Clearly the window of opportunity for fertility is considerably reduced in this age group. Odeblad has also shown that pregnancy increases the growth of S mucus crypts, hence, multiple pregnancies will maintain fertility until an older age is reached. When the cervix has aged, a woman may ovulate, but produce no cervical mucus even though she may have a biphasic temperature. Since the mucus is essential for sperm entry, such women are said to have non-fertile ovulations. A study of 138 premenopausal women found no pregnancies beyond the age of 45; the method-related pregnancy rate at 40-44 years of age was 0 32% and the informed choice pregnancy rate was 1 6%.
Discontinuation of Ovulation Suppression
The return to fertility after discontinuation of ovulation suppressants varies from immediate resumption of previous patterns to post-pill amenorrhea. If the woman is going to ovulate, she will find a mucus build up followed by biphasic temperatures. The cervical eversion which is found in at least 25 percent of women who have used the birth control pill for over 3 months weeps copious amounts of fertile-type mucus once the woman stops ingesting progestins. It is not unusual to find 14 days of slippery, stretchy, clear mucus in the first off-pill cycle. Experience has shown that if the number of mucus days do not decrease considerably by the third cycle, cryosurgery or silver nitrate treatment after cytologic and colposcopic studies have shown no other pathology, is appropriate and curative. Care must be taken not to confuse the normal eversion of the preovulatory cervix with persistent effect of the "pill." It is also important to freeze only the glandular epithelium on the portio vaginalis, and not destroy the normal endocervix. Excess freezing or hot cautery can destroy the mucus producing crypts, as can a high conization. While a cervical eversion is weeping mucus, a woman may not be able to distinguish her peak symptom, particularly if she has had no prior experience. Monitoring BBT at least initially may help build confidence.
Cervicitis and Vaginitis
Any woman who knows her fertility pattern will detect an abnormality quickly and seek treatment. Chronic baseline discharge is readily distinguished from the buildup pattern. Local medication may mask mucus (as do contraceptive foams and gels). If the pattern cannot be perceived, and the couple do not wish to risk a pregnancy, they must abstain until their pattern becomes recognizable. Trichomoniasis and bacterial vaginosis will alter the normal pattern and require appropriate treatment.
With systemic or local antibiotic treatment, monilial vaginitis is common, and may obscure the mucus pattern; abstinence must be advised until the pattern clears, if pregnancy avoidance is desired. Antihistamines tend to thicken mucus, while guafenisin liquifies it. Cervicitis may produce an "inflammatory mucus" similar in structure to G mucus.
Ovulation Suppression by Stress and Pharmaceuticals
The role of physical and emotional stress in suppressing ovulation via alteration of the hypothalamopituitary axis is well-known and well documented. Sudden weight loss, environmental stress and/or change, have led to amenorrhea. When stress suppresses ovulation, a pattern of intermittent mucus without a peak is seen. Such a cycle is, of course, monophasic, and shows no increase in progesterone. Often the emotionally or physically stressful events are easily correlated with the mucus patterns, and resolution of conflict is then followed by (delayed) ovulation. McArthur et al. found that in three women who recently began running, the amenorrhea was associated with normal body composition, low baseline concentrations of LH and normal concentrations of FSH, normal to hyperresponsiveness of LH and FSH to GnRH testing, and normal and possibly increased frequency of LH pulsations. They believe that an alteration in the hypothalamic control of gonadotropin release, independent of body composition, is operant in the development of "athletic amenorrhea." While mucus observations were not made in these women, vaginal cytohormonal studies indicated moderate vaginal atrophy. Taylor et al. have correlated the highest karyopyknotic index with the peak mucus symptom and found close correlations to date.
The use of psychotropic drugs, particularly the phenothiazines, is associated with amenorrhea and, at times, with inappropriate lactation, presumably as a result of prolactin increase. In such women, the normal ovulatory mucus pattern is disturbed and can signal the disturbed hormonal picture. There are anecdotal reports of ovulation suppression following tetrahydrocannabinol (THC) smoking, as reflected in the mucus patterns. While ovulation disturbances are seen in hard drug users, they are difficult to define due to erratic use (they are known to become pregnant) and are not easily separated out from their dietary confounding factors. Any systemic illness which interferes with ovulation, i.e., hypo- or hyperthyroidism, will be reflected in the mucus and thermal patterns.
Biochemical Indicators of Fertility
Various monitoring devices have been used to correlate physiological fertility signs with hormonal parameters. Some devices are teaching aids or are used to clarify a difficult mucus pattern while others are being marketed as "less subjective" than self detection of mucus. Still other devices measure vaginal fluid volume, or program calendar rhythm data, thermal shifts, and mucus patterns into computers. Most devices attempt to identify the beginning and end of the fertile phase, among them home monitors which detect the oestrogen rise which marks the beginning of fertility and those which detect the rise of progesterone at the end of fertility. WHO has supported field testing of several monitors, J. Brown's assay is among the most widely tested. The Brown Ovarian monitor utilizes a micrococcus enzyme immunoassay to measure the levels of oestradiol and progesterone metabolites in the urine (oestrone glucuronide [E1G] and pregnanediol glucuronide [PdG]). Another monitor uses an expensive device to monitor urine oestrogen and LH surge. The average number of fertile days obtained:
NFP Method ---------- Ave. No. Fertile Days
Ovarian Monitor ----- 8.9
Ovulation Method ---- 10.4
Sympto-thermal ------ 11.8
Bioself 110 --------- 15.0
Persona ------------ 6-12 (7)
Dipsticks for LH surge which identify the impending LH surge 72 hours in advance can assist couples who are seeking to achieve pregnancy. LH monitors cannot be used for pregnancy avoidance, as most women have more than 2 days of mucus before peak, and sperm will remain viable in mucus for more than 3 days. Since it is the mucus and not the hormone that serves as the gatekeeper for the sperm, it is never prudent to ignore the mucus sign. To date, none of the devices except the Brown ovarian monitor have duplicated the radio-immune assayed plasma hormonal levels. In clinical trials the unplanned pregnancy rates were 5-10%.
Next Page:
Couple Autonomy
1,
2
Article copyrights are held solely by author.
[ Japan-Lifeissues.net ] [ OMI Japan/Korea ]